Business Name: BeeHive Homes Assisted Living
Address: 16220 West Rd, Houston, TX 77095
Phone: (832) 906-6460
BeeHive Homes Assisted Living
BeeHive Homes Assisted Living of Cypress offers assisted living and memory care services in a warm, comfortable, and residential setting. Our care philosophy focuses on personalized support, safety, dignity, and building meaningful connections for each resident. Welcoming new residents from the Cypress and surrounding Houston TX community.
16220 West Rd, Houston, TX 77095
Business Hours
Monday thru Sunday: 7:00am - 7:00pm
Facebook: https://www.facebook.com/BeeHiveHomesCypress
Moving a parent or partner from the home they like into senior living is seldom a straight line. It is a braid of feelings, logistics, finances, and family dynamics. I have walked households through it during medical facility discharges at 2 a.m., during peaceful kitchen-table talks after a near fall, and throughout urgent calls when roaming or medication errors made staying home hazardous. No 2 journeys look the same, but there are patterns, common sticking points, and practical ways to relieve the path.
This guide draws on that lived experience. It will not talk you out of concern, but it can turn the unknown into a map you can check out, with signposts for assisted living, memory care, and respite care, and useful concerns to ask at each turn.
The emotional undercurrent nobody prepares you for
Most households anticipate resistance from the elder. What surprises them is their own resistance. Adult kids typically tell me, "I guaranteed I 'd never ever move Mom," only to discover that the guarantee was made under conditions that no longer exist. When bathing takes 2 people, when you discover unpaid bills under sofa cushions, when your dad asks where his long-deceased brother went, the ground shifts. Guilt comes next, in addition to relief, which then sets off more guilt.
You can hold both realities. You can like someone deeply and still be not able to meet their needs at home. It helps to call what is happening. Your role is altering from hands-on caretaker to care planner. That is not a downgrade in love. It is a change in the sort of help you provide.
Families often fret that a relocation will break a spirit. In my experience, the broken spirit normally comes from persistent exhaustion and social seclusion, not from a new address. A little studio with stable routines and a dining room filled with peers can feel bigger than an empty house with 10 rooms.
Understanding the care landscape without the marketing gloss
"Senior care" is an umbrella term that covers a spectrum. The best fit depends on needs, choices, spending plan, and location. Think in regards to function, not labels, and take a look at what a setting actually does day to day.
Assisted living supports day-to-day jobs like bathing, dressing, medication management, and meals. It is not a medical center. Residents reside in homes or suites, frequently bring their own furniture, and participate in activities. Laws vary by state, so one building may deal with insulin injections and two-person transfers, while another will not. If you need nighttime assistance regularly, verify staffing ratios after 11 p.m., not simply throughout the day.
Memory care is for people dealing with Alzheimer's or other types of dementia who require a safe environment and specialized programming. Doors are secured for safety. The best memory care units are not just locked hallways. They have trained personnel, purposeful routines, visual hints, and enough structure to lower anxiety. Ask how they manage sundowning, how they respond to exit-seeking, and how they support locals who resist care. Try to find evidence of life enrichment that matches the person's history, not generic activities.
Respite care describes short stays, typically 7 to 30 days, in assisted living or memory care. It gives caregivers a break, offers post-hospital healing, or functions as a trial run. Respite can be the bridge that makes a permanent move less complicated, for everyone. Policies vary: some communities keep the respite resident in a supplied apartment or condo; others move them into any available system. Validate everyday rates and whether services are bundled or a la carte.
Skilled nursing, frequently called nursing homes or rehabilitation, supplies 24-hour nursing and treatment. It is a medical level of care. Some seniors release from a hospital to short-term rehab after a stroke, fracture, or severe infection. From there, families choose whether going back home with services is practical or if long-term positioning is safer.

Adult day programs can support life at home by providing daytime guidance, meals, and activities while caregivers work or rest. They can decrease the threat of seclusion and give structure to an individual with amnesia, often delaying the requirement for a move.
When to begin the conversation
Families typically wait too long, requiring choices throughout a crisis. I try to find early signals that recommend you must at least scout choices:
- Two or more falls in 6 months, specifically if the cause is unclear or involves bad judgment instead of tripping. Medication errors, like duplicate dosages or missed out on necessary meds a number of times a week. Social withdrawal and weight loss, frequently signs of anxiety, cognitive modification, or difficulty preparing meals. Wandering or getting lost in familiar locations, even once, if it includes safety threats like crossing hectic roads or leaving a range on. Increasing care needs in the evening, which can leave family caretakers sleep-deprived and vulnerable to burnout.
You do not need to have the "relocation" discussion the very first day you discover issues. You do require to unlock to planning. That might be as basic as, "Dad, I 'd like to visit a couple places together, just to know what's out there. We won't sign anything. I want to honor your preferences if things alter down the road."
What to search for on tours that brochures will never ever show
Brochures and websites will reveal bright spaces and smiling homeowners. The genuine test is in unscripted minutes. When I tour, I get here 5 to ten minutes early and view the lobby. Do groups greet locals by name as they pass? Do locals appear groomed, or do you see unbrushed hair and untied shoes at 10 a.m.? Notice smells, however interpret them fairly. A short odor near a restroom can be regular. A persistent smell throughout common locations signals understaffing or bad housekeeping.
Ask to see the activity calendar and after that try to find evidence that occasions are really happening. Exist supplies on the table for the scheduled art hour? Exists music when the calendar states sing-along? Speak with the citizens. Many will tell you honestly what they enjoy and what they miss.
The dining-room speaks volumes. Demand to eat a meal. Observe the length of time it requires to get served, whether the food is at the ideal temperature level, and whether staff help quietly. If you are thinking about memory care, ask how they adjust meals for those who forget to eat. Finger foods, contrasting plate colors, and shorter, more regular offerings can make a big difference.
Ask about over night staffing. Daytime ratios frequently look sensible, but numerous communities cut to skeleton crews after supper. If your loved one requires frequent nighttime help, you require to know whether two care partners cover an entire flooring or whether a nurse is offered on-site.
Finally, view how management handles concerns. If they answer without delay and transparently, they will likely address problems by doing this too. If they dodge or sidetrack, expect more of the exact same after move-in.
The monetary labyrinth, simplified enough to act
Costs differ extensively based upon geography and level of care. As a rough variety, assisted living often runs from $3,000 to $7,000 per month, with additional fees for care. Memory care tends to be higher, from $4,500 to $9,000 per month. Knowledgeable nursing can go beyond $10,000 monthly for long-term care. Respite care normally charges an everyday rate, frequently a bit greater per day than an irreversible stay since it includes home furnishings and flexibility.
Medicare does not spend for custodial care in assisted living or memory care. It covers medical services, hospitalizations, and short-term rehabilitation if criteria are satisfied. Long-term care insurance coverage, if you have it, might cover part of assisted living or memory care when you fulfill advantage triggers, normally measured by needs in activities of daily living or recorded cognitive disability. Policies vary, so check out the language carefully. Veterans might receive Aid and Presence advantages, which can balance out costs, but approval can take months. Medicaid covers long-lasting care for those who satisfy monetary and scientific requirements, often in nursing homes and, in some states, in assisted living through waiver programs. Waiting lists exist. Talk early with a local elder law lawyer if Medicaid may belong to your strategy in the next year or two.
Budget for the concealed items: move-in costs, second-person charges for couples, cable television and web, incontinence materials, transport charges, hairstyles, and increased care levels in time. It prevails to see base lease plus a tiered care plan, however some communities use a point system or flat all-encompassing rates. Ask how frequently care levels are reassessed and what typically sets off increases.
Medical realities that drive the level of care
The distinction in between "can remain at home" and "requires assisted living or memory care" is typically medical. A few examples highlight how this plays out.
Medication management appears little, however it is a big driver of security. If someone takes more than 5 daily medications, particularly consisting of insulin or blood slimmers, the risk of error increases. Pill boxes and alarms help until they do not. I have actually seen individuals double-dose since the box was open and they forgot they had actually taken the pills. In assisted living, staff can cue and administer medications on a set schedule. In memory care, the approach is frequently gentler and more consistent, which individuals with dementia require.
Mobility and transfers matter. If someone needs 2 individuals to transfer safely, lots of assisted livings will decline them or will require private aides to supplement. An individual who can pivot with a walker and one steadying arm is typically within assisted living ability, specifically if they can bear weight. If weight-bearing is poor, or if there is uncontrolled habits like starting out throughout care, memory care or skilled nursing may be necessary.
Behavioral signs of dementia dictate fit. Exit-seeking, substantial agitation, or late-day confusion can be better managed in memory care with environmental hints and specialized staffing. When a resident wanders into other houses or withstands bathing with yelling or hitting, you are beyond the capability of a lot of general assisted living teams.
Medical devices and competent requirements are a dividing line. Wound vacs, intricate feeding tubes, regular catheter irrigation, or oxygen at high circulation can push care into skilled nursing. Some assisted livings partner with home health firms to bring nursing in, which can bridge care for specific requirements like dressing modifications or PT after a fall. Clarify how that coordination works.
A humane move-in plan that actually works
You can reduce tension on relocation day by staging the environment first. Bring familiar bedding, the preferred chair, and photos for the wall before your loved one gets here. Set up the home so the course to the restroom is clear, lighting is warm, and the very first thing they see is something soothing, not a stack of boxes. Label drawers and closets in plain language. For memory care, eliminate extraneous products that can overwhelm, and place hints where they matter most, like a large clock, a calendar with household birthdays marked, and a memory shadow box by the door.
Time the move for late morning or early afternoon when energy tends to be steadier. Avoid late-day arrivals, which can collide with sundowning. Keep the group small. Crowds of relatives ramp up anxiety. Choose ahead who will stay for the first meal and who will leave after assisting settle. There is no single right response. Some people do best when family stays a number of hours, takes part in an activity, and returns the next day. Others transition much better when household leaves after greetings and personnel step in with a meal or a walk.
Expect pushback and plan for it. I have heard, "I'm not staying," sometimes on move day. Staff trained in dementia care will reroute rather than argue. They may recommend a tour of the garden, introduce a welcoming resident, or invite the new person into a preferred activity. Let them lead. If you go back for a few minutes and enable the staff-resident relationship to form, it often diffuses the intensity.
Coordinate medication transfer and doctor orders before relocation day. Lots of communities need a doctor's report, TB screening, signed medication orders, and a list of allergic reactions. If you wait until the day of, you risk hold-ups or missed out on doses. Bring two weeks of medications in initial pharmacy-labeled containers unless the community uses a particular packaging vendor. Ask how the transition to their pharmacy works and whether there are delivery cutoffs.
The first thirty days: what "settling in" truly looks like
The very first month is a change period for everybody. Sleep can be interfered with. Appetite might dip. Individuals with dementia might ask to go home consistently in the late afternoon. This is regular. Foreseeable routines help. Encourage involvement in 2 or 3 activities that match the individual's interests. A woodworking hour or a small walking club is more effective than a jam-packed day of occasions somebody would never ever have picked before.
Check in with staff, however resist the urge to micromanage. Ask for a care conference at the two-week mark. Share what you are seeing and ask what they are observing. You might learn your mom consumes better at breakfast, so the team can pack calories early. Or that your dad sunbathes by the window and enjoys it more than bingo, so personnel can construct on that. When a resident refuses showers, staff can try varied times or use washcloth bathing until trust forms.
Families often ask whether to visit daily. It depends. If your existence calms the individual and they engage with the neighborhood more after seeing you, visit. If your check outs trigger upset or demands to go home, space them out and collaborate with staff on timing. Short, consistent gos to can be better than long, occasional ones.
Track the little wins. The very first time you get an image of your father smiling at lunch with peers, the day the nurse contacts us to say your mother had no lightheadedness after her early morning medications, the night you sleep 6 hours in a row for the first time in months. These are markers that the decision is bearing fruit.
Respite care as a test drive, not a failure
Using respite care can feel like you are sending someone away. I have actually seen the opposite. A two-week stay after a health center discharge can prevent a quick readmission. A month of respite while you recover from your own surgery can secure your health. And a trial remain answers genuine questions. Will your mother accept help with bathing more quickly from staff than from you? Does your father eat better when he is not eating alone? Does the sundowning minimize when the afternoon includes a structured program?
If respite goes well, the move to long-term residency ends up being much easier. The house feels familiar, and staff currently know the individual's rhythms. If respite reveals a poor fit, you discover it without a long-lasting commitment and can try another neighborhood or change the strategy at home.
When home still works, but not without support
Sometimes the best answer is not a move right now. Maybe your house is single-level, the elder remains socially linked, and the dangers are workable. In those cases, I try to find 3 supports that keep home practical:
- A reliable medication system with oversight, whether from a checking out nurse, a clever dispenser with alerts to household, or a drug store that packages meds by date and time. Regular social contact that is not depending on a single person, such as adult day programs, faith neighborhood sees, or a next-door neighbor network with a schedule. A fall-prevention strategy that includes getting rid of rugs, adding grab bars and lighting, making sure shoes fits, and scheduling balance exercises through PT or community classes.
Even with these supports, revisit the plan every 3 to 6 months or after any hospitalization. Conditions alter. Vision intensifies, arthritis flares, memory decreases. At some point, the equation will tilt, and you will be pleased you already scouted assisted living or memory care.
Family characteristics and the hard conversations
Siblings frequently hold different views. One may push for staying at home with more help. Another fears the next fall. A third lives far away and feels guilty, which can sound like criticism. I have actually found it handy to externalize the decision. Rather of arguing viewpoint versus opinion, anchor the conversation to 3 concrete pillars: security occasions in the last 90 days, practical status measured by daily jobs, and caregiver capability in hours each week. Put numbers on paper. If Mom needs 2 hours of aid in the morning and 2 at night, 7 days a week, that is 28 hours. If those hours are beyond what household can offer sustainably, the options narrow to working with in-home care, adult day, or a move.
Invite the elder into the conversation as much as possible. Ask what matters most: hugging a certain friend, keeping an animal, being close to a particular park, eating a specific cuisine. If a move is needed, you can use those choices to select the setting.
Legal and practical foundation that avoids crises
Transitions go smoother when documents are all set. Durable power of lawyer and health care proxy must remain in place before cognitive decrease makes them difficult. If dementia exists, get a physician's memo documenting decision-making capacity at the time of signing, in case anybody questions it later. A HIPAA release enables staff to share essential info with designated family.
Create a one-page medical snapshot: medical diagnoses, medications with dosages and schedules, allergies, main physician, professionals, current hospitalizations, and standard performance. Keep it upgraded and printed. Hand it to emergency department personnel if required. Share it with the senior living nurse on move-in day.
Secure valuables now. Move precious jewelry, delicate files, and nostalgic products to a safe location. In common memory care settings, small items go missing out on for innocent factors. Avoid heartbreak by removing temptation and confusion before it happens.
What good care feels like from the inside
In exceptional assisted living and memory care communities, you feel a rhythm. Early mornings are busy but not frenzied. Personnel speak with locals at eye level, with heat and regard. You hear laughter. You see a resident who when slept late signing up with a workout class due to the fact that someone continued with mild invites. You observe staff who know a resident's preferred song or the way he likes his eggs. You observe versatility: shaving can wait until later if somebody is grumpy at 8 a.m.; the walk can happen after coffee.
Problems still occur. A UTI activates delirium. A medication triggers dizziness. A resident grieves the loss of driving. The difference remains in the response. Great teams call quickly, include the household, change the plan, and follow up. They do not pity, they do not conceal, and they do not default to restraints or sedatives without careful thought.
The truth of modification over time
Senior care is not a fixed choice. Requirements develop. An individual might move into assisted living and do well for 2 years, then establish wandering or nighttime confusion that requires memory care. Or they may thrive in memory look after a long stretch, then develop medical problems that press toward knowledgeable nursing. Spending plan for these shifts. Mentally, prepare for them too. The 2nd move can be much easier, due to the fact that the group often helps and the family currently knows the terrain.
I have actually likewise seen the reverse: individuals who enter memory care and support so well that habits diminish, weight improves, and the need for intense interventions drops. When life is structured and calm, the brain does better with the resources it has actually left.
Finding your footing as the relationship changes
Your task changes when your loved one moves. You become historian, advocate, and companion rather than sole caretaker. Visit with purpose. Bring stories, pictures, music playlists, a favorite lotion for a hand massage, or a basic project you can do together. Join an activity now and then, not to remedy it, but to experience their day. Find out the names of the care partners and nurses. A simple "thank you," a vacation card with pictures, or a box of cookies goes even more than you think. Staff are human. Valued teams do much better work.
Give yourself time to grieve the old regular. It is suitable to feel loss and relief at the very same time. Accept help on your own, whether from a caregiver support system, a therapist, or a good friend who can handle the documentation at your cooking area table when a month. Sustainable caregiving includes take care of the caregiver.
A short checklist you can in fact use
- Identify the current leading 3 threats in the house and how typically they occur. Tour a minimum of two assisted living or memory care neighborhoods at different times of day and eat one meal in each. Clarify overall monthly expense at each option, consisting of care levels and most likely add-ons, and map it against a minimum of a two-year horizon. Prepare medical, legal, and medication documents 2 weeks before any prepared move and confirm pharmacy logistics. Plan the move-in day with familiar items, simple routines, and a small assistance group, then set up a care conference two weeks after move-in.
A course forward, not a verdict
Moving from home to senior living is not about giving up. It has to do with building a new support group around an individual you love. Assisted living can bring back energy and neighborhood. Memory care can make life much safer and calmer when the brain misfires. Respite care can offer a bridge and a breath. Good elderly care honors a person's history while adapting to their present. If you approach the transition with clear eyes, constant planning, and a willingness to let specialists bring a few of the weight, you produce space for something lots of families have not felt in a long period of time: a more serene everyday.
BeeHive Homes Assisted Living is an Assisted Living Facility
BeeHive Homes Assisted Living is an Assisted Living Home
BeeHive Homes Assisted Living is located in Cypress, Texas
BeeHive Homes Assisted Living is located Northwest Houston, Texas
BeeHive Homes Assisted Living offers Memory Care Services
BeeHive Homes Assisted Living offers Respite Care (short-term stays)
BeeHive Homes Assisted Living provides Private Bedrooms with Private Bathrooms for their senior residents
BeeHive Homes Assisted Living provides 24-Hour Staffing
BeeHive Homes Assisted Living serves Seniors needing Assistance with Activities of Daily Living
BeeHive Homes Assisted Living includes Home-Cooked Meals Dietitian-Approved
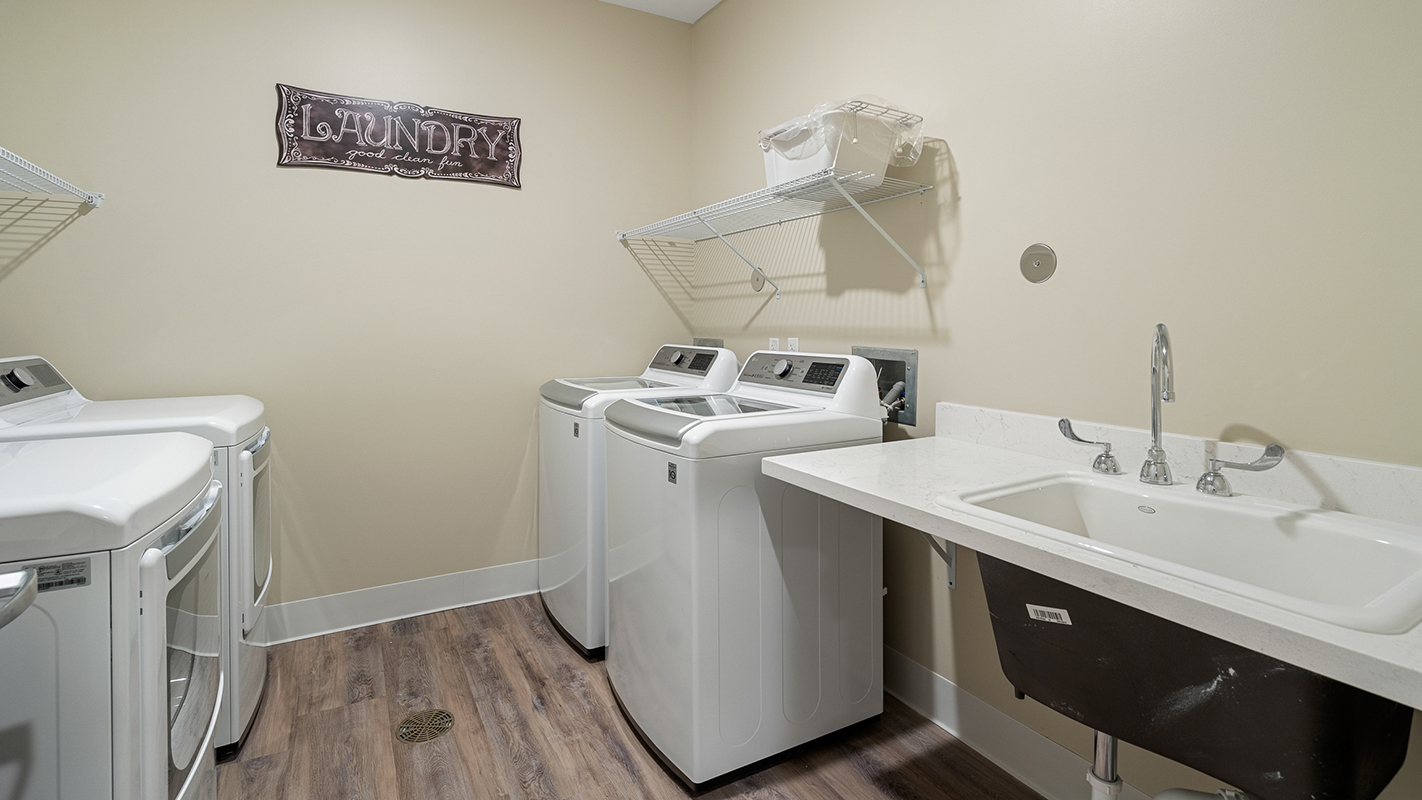
BeeHive Homes Assisted Living includes Daily Housekeeping & Laundry Services
BeeHive Homes Assisted Living features Private Garden and Green House
BeeHive Homes Assisted Living has a Hair/Nail Salon on-site
BeeHive Homes Assisted Living has a phone number of (832) 906-6460
BeeHive Homes Assisted Living has an address of 16220 West Road, Houston, TX 77095
BeeHive Homes Assisted Living has website https://beehivehomes.com/locations/cypress
BeeHive Homes Assisted Living has Google Maps listing https://maps.app.goo.gl/G6LUPpVYiH79GEtf8
BeeHive Homes Assisted Living has Facebook page https://www.facebook.com/BeeHiveHomesCypress
BeeHive Homes Assisted Living is part of the brand BeeHive Homes
BeeHive Homes Assisted Living focuses on Smaller, Home-Style Senior Residential Setting
BeeHive Homes Assisted Living has care philosophy of “The Next Best Place to Home”
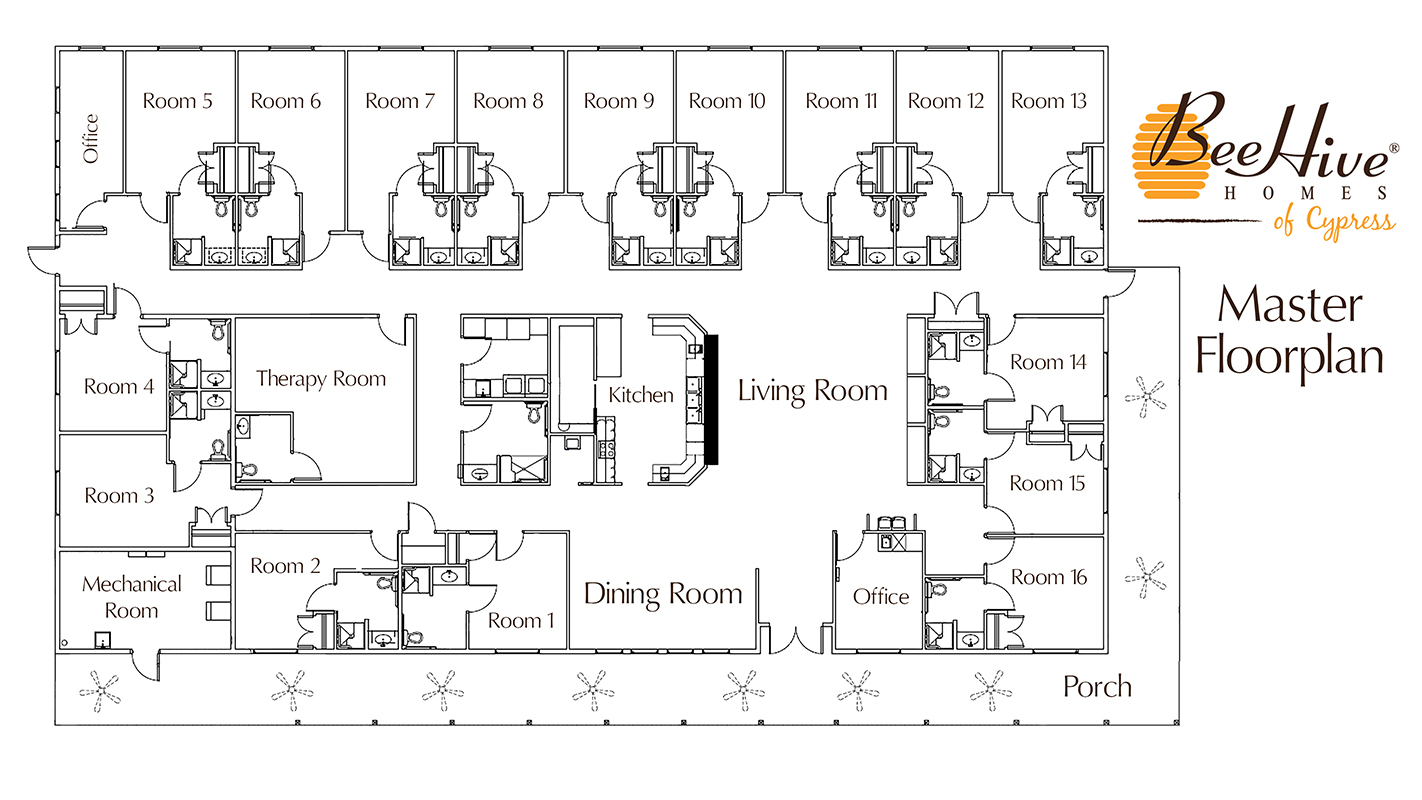
BeeHive Homes Assisted Living has floorplan of 16 Private Bedrooms with ADA-Compliant Bathrooms
BeeHive Homes Assisted Living welcomes Families for Tours & Consultations
BeeHive Homes Assisted Living promotes Engaging Activities for Senior Residents
BeeHive Homes Assisted Living emphasizes Personalized Care Plans for each Resident
BeeHive Homes Assisted Living won Top Branded Assisted Living Houston 2025
BeeHive Homes Assisted Living earned Outstanding Customer Service Award 2024
BeeHive Homes Assisted Living won Excellence in Assisted Living Homes 2023
People Also Ask about BeeHive Homes Assisted Living
What services does BeeHive Homes Assisted Living of Cypress provide?
BeeHive Homes Assisted Living of Cypress provides a full range of assisted living and memory care services tailored to the needs of seniors. Residents receive help with daily activities such as bathing, dressing, grooming, medication management, and mobility support. The community also offers home-cooked meals, housekeeping, laundry services, and engaging daily activities designed to promote social interaction and cognitive stimulation. For individuals needing specialized support, the secure memory care environment provides additional safety and supervision.
How is BeeHive Homes Assisted Living of Cypress different from larger assisted living facilities?
BeeHive Homes Assisted Living of Cypress stands out for its small-home model, offering a more intimate and personalized environment compared to larger assisted living facilities. With 16 residents, caregivers develop deeper relationships with each individual, leading to personalized attention and higher consistency of care. This residential setting feels more like a real home than a large institution, creating a warm, comfortable atmosphere that helps seniors feel safe, connected, and truly cared for.
Does BeeHive Homes Assisted Living of Cypress offer private rooms?
Yes, BeeHive Homes Assisted Living of Cypress offers private bedrooms with private or ADA-accessible bathrooms for every resident. These rooms allow individuals to maintain dignity, independence, and personal comfort while still having 24-hour access to caregiver support. Private rooms help create a calmer environment, reduce stress for residents with memory challenges, and allow families to personalize the space with familiar belongings to create a “home-within-a-home” feeling.
Where is BeeHive Homes Assisted Living located?
BeeHive Homes Assisted Living is conveniently located at 16220 West Road, Houston, TX 77095. You can easily find direction on Google Maps or visit their home during business hours, Monday through Sunday from 7am to 7pm.
How can I contact BeeHive Homes Assisted Living?
You can contact BeeHive Assisted Living by phone at: 832-906-6460, visit their website at https://beehivehomes.com/locations/cypress/, or connect on social media via Facebook
Looking for assisted living near fun shopping? We are located near The Boardwalk at Towne Lake.